Summer Adventures Start With Smart Preparation
The trails are busy, the rivers are rushing, and the wilderness is calling. July is the perfect time to level up your training and refresh your decision-making tools.
In this month’s newsletter, meet Instructor Micaela Klutz and learn what fuels her passion for teaching in remote settings. Plus, dive into Part 2 of last month’s case study and see how the scenario develops.
From the field to the classroom, we’re here to help you stay prepared—no matter where your summer takes you.
SURVEY
Your Feedback on Learning Materials
At WMA International, we’re committed to enhancing your learning experience. To better understand your preferences, we invite you to participate in a 4-question survey regarding the format of our field guides, SOAP notes, and textbooks. Your input will help us determine whether printed or digital materials are most suitable for your learning needs. Thank you for sharing your feedback with us!
COURSE SPOTLIGHT
Hey Maine-ahs! Is it time to recertify your Wilderness First Responder?
Your Wilderness First Responder certification is only valid for three years—don’t let it lapse! A WFR Recertification course is designed to refresh your hands-on skills, reinforce decision-making in remote settings, and update your knowledge with the latest protocols in wilderness medicine.
We’ve got two upcoming WFR Recertification courses in Maine to help you get recertified:
Hybrid WFR Recertification | August 31 – September 1, 2025 | Spruce Head, ME
Hosted by Hurricane Island Outward Bound and taught by Abby Rowe, President of Wilderness Medical Associates International, this hybrid option combines online pre-course work with two immersive days on the coast of Maine.
WFR Recertification | September 26–28, 2025 | Freeport, ME
A fully in-person, three-day course hosted by L.L. Bean, facilitated by Healing All Wounds, LLC.
Recertify where the pines meet the sea—join us in Maine. Click the buttons below to learn more or to register now!
INSTRUCTOR SPOTLIGHT
Micaela Klutz
Micaela Klutz didn’t set out to become a wilderness medicine instructor—but sometimes, the best adventures are the unplanned ones. With a background in guiding and a deep love for the outdoors, Micaela took a leap when she saw an opportunity to train with Wilderness Medical Associates. “I just thought, I’ll give it a shot and see what I think,” she recalls. “And the more I taught, the more I fell in love with it.”
Based in Canmore, Alberta, Micaela is a paramedic who brings years of guiding and outdoor experience to her WMA teaching. She currently manages and guides for a local whitewater rafting
company, teaches Swiftwater rescue courses, and has worked in a variety of outdoor-related roles including ski patrol. When Micaela is not teaching WMA courses, you’ll likely find her kayaking, hiking, or diving into yet another outdoor job.

Live from the Wild
The latest shares from WMA International students & instructors!



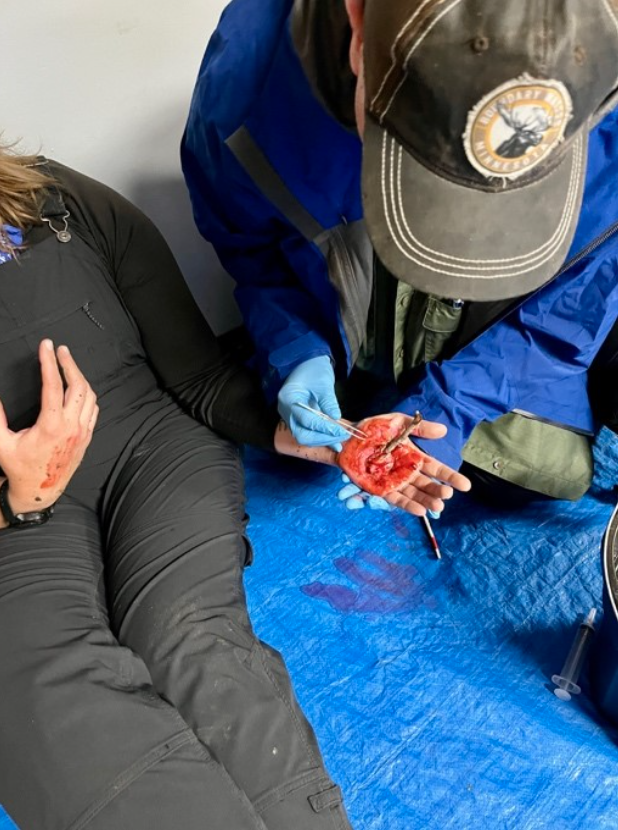
CASE STUDY
Part 2: Canoeing, North Woods, Maine Summer 2025
In our last newsletter, we met a canoeist paddling in the North Maine Woods who was feeling unusually run down, feverish, and had a concerning rash on his lower back. You can review the case here.
Let’s move on to the assessment, anticipated problems, and treatment plan:

Discussion:
This is a serious problem, even if you’re not certain what it is. If we consider the principle of approaching problems from “generic to specific,” we see that there are signs of a local spreading infection (redness, warmth, swelling) and signs of a concerning systemic infection (fever, subdued personality). Either way, this case has progressed to require treatment beyond what we can provide in the field. If it’s a systemic infection, or a tick-borne illness (in this case, disseminated Lyme Disease from an embedded Deer Tick is the most concerning tick-borne illness that is consistent with this presentation), treatment with selective antibiotics will be much more effective the earlier they are given. Getting out sooner will make a difference in their care and success in the long run.
One of the most important parts of care is to remove the entire offending tick (and any others) and perform wound cleaning. Use fine-edge tweezers to get under the head and mouthparts of the tick, deliberately pulling out the entire tick without squeezing its body. Home remedies like petroleum jelly, burnt match ends, and nail polish don’t remove the tick or its contaminated mouthparts.
Tick identification can help with some problem-solving. Keep in mind that there are many types of ticks out there, and their endemic ranges are growing. This is a reminder to approach your problem-solving with a “big net.” There are many tick-borne diseases to consider in addition to Lyme Disease. STARI (Southern Tick-Associated Rash Illness), spread by the Lone-Star tick mimics many symptoms of Lyme.
And of course, people travel from one region to another, perhaps unaware of their parasitic tagalong. One of our instructors treated a case of advanced Rocky Mountain Spotted Fever in rural Alaska.
Would you like to learn more about tick-borne illness and current treatment? Here are some websites to check out:
University of Rhode Island Tick Encounter
FAQs about Ticks and Mosquitos from State of Maine
Maine Tracking Data for Tickborne Diseases
Send us photos from your course!
We’d love to see the behind-the-scenes of your experience.
